Governance Pyramid
The Governance Pyramid in Healthcare
A Practical Guide to Strengthening Governance in Healthcare Organizations
Introduction
Healthcare organizations operate in complex environments where patient safety, quality of care, financial sustainability, and accountability must all be managed simultaneously. Effective governance provides the structure through which these responsibilities are coordinated, monitored, and improved.
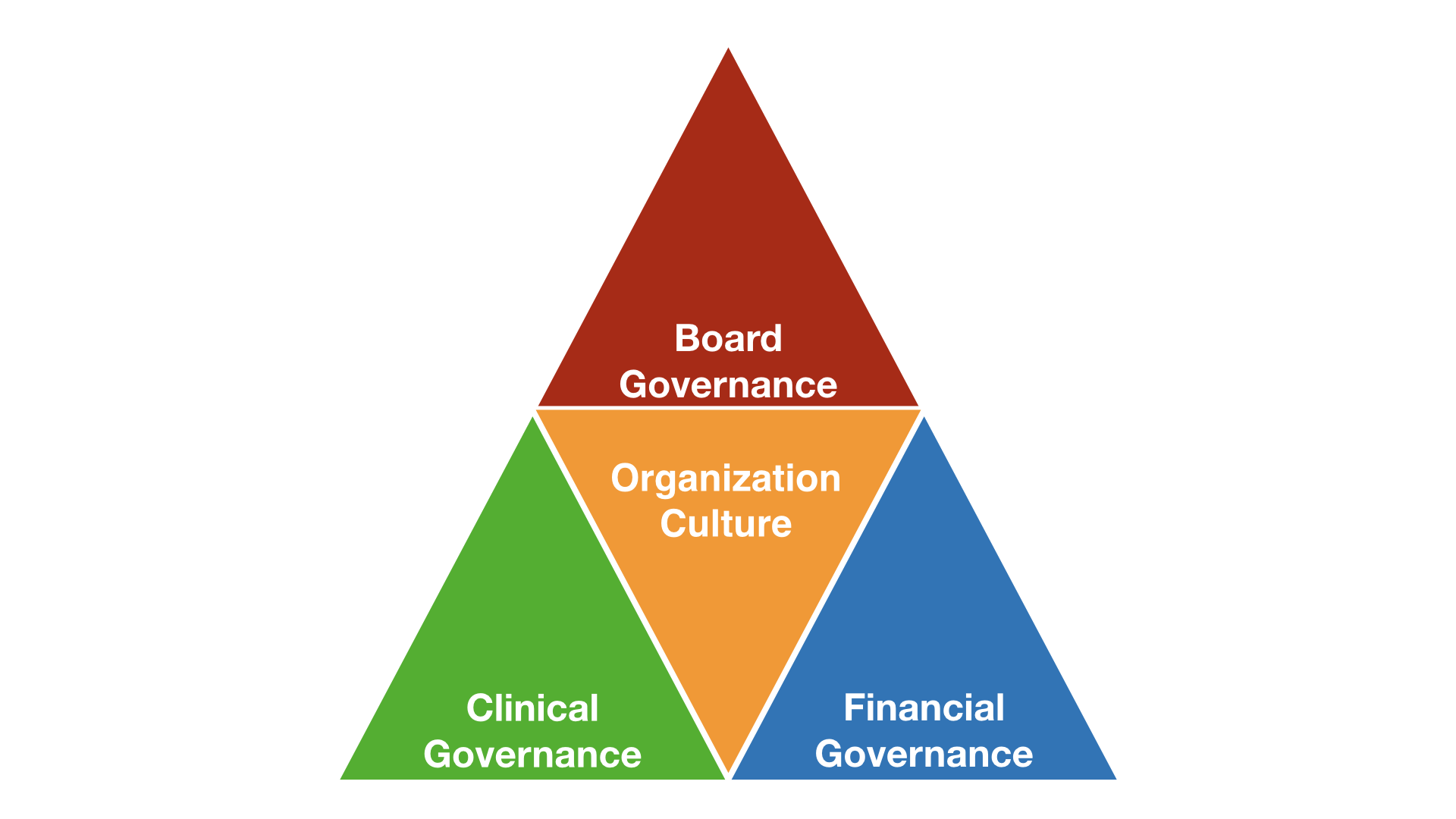
One useful way to conceptualize governance in healthcare is through the Governance Pyramid. This model represents the essential elements that support sound governance within a healthcare organization. At the top of the pyramid lies Board Governance, which provides strategic leadership and oversight. At the base of the pyramid lie Clinical Governance and Financial Governance, which ensure that healthcare delivery is safe, effective, and sustainable. Binding these elements together is the organizational culture, which reflects the principles of good governance—such as transparency, accountability, participation, integrity, and continuous improvement.
The Governance Pyramid offers a structured way to understand how leadership, systems, and values interact to support high-performing healthcare organizations.
Understanding the Governance Pyramid
The governance pyramid illustrates three interrelated levels of governance:
-
- Board Governance (Strategic Level)
- Clinical Governance (Quality and Safety Level)
- Financial Governance (Resource Stewardship Level)
Although these elements can be described separately, they operate as an integrated system. When aligned and supported by a strong organizational culture, they promote accountability, safety, efficiency, and trust within healthcare organizations.
Board Governance: Strategic Leadership at the Top
At the top of the governance pyramid sits Board Governance, representing the highest level of oversight within a healthcare organization. The governing board—often called the Board of Directors, Board of Trustees, or Governing Council—is responsible for ensuring that the organization fulfills its mission, operates ethically, and delivers value to patients and the community. Key roles of board governance include:
1. Strategic Direction
The board sets the long-term vision and strategic priorities of the organization. This includes defining goals related to:
-
- Quality of care
- Patient safety
- Organizational growth
- Community health impact
- Financial sustainability
By setting a clear strategic direction, the board ensures that the organization remains aligned with its mission and values.
2. Accountability and Oversight
Boards ensure that executive leadership is accountable for performance. This oversight includes monitoring:
-
- Clinical outcomes
- Patient safety indicators
- Financial performance
- Compliance with laws and regulations
- Risk management activities
Through regular reporting and performance review, the board ensures that the organization maintains high standards.
3. Policy and Governance Framework
The board establishes the policies and governance structures that guide organizational operations. These policies define:
-
- Ethical standards
- Decision-making processes
- Roles and responsibilities
- Risk management frameworks
Strong policies ensure clarity, fairness, and consistency across the organization.
4. Leadership and Stewardship
Board members act as stewards of the organization’s mission. They represent the interests of patients, staff, and the broader community. By promoting transparency, integrity, and ethical leadership, the board sets the tone for the entire organization.
Clinical Governance: Ensuring Quality and Patient Safety
One of the foundational pillars at the base of the governance pyramid is Clinical Governance. Clinical governance refers to the system through which healthcare organizations are accountable for continuously improving the quality of their services and safeguarding high standards of patient care. It ensures that patients receive care that is safe, effective, patient-centered, timely, efficient, and equitable. Clinical governance includes several interrelated components:
1. Clinical Effectiveness
Clinical effectiveness ensures that healthcare interventions are based on the best available evidence. Key mechanisms include:
-
- Evidence-based clinical guidelines
- Clinical audits
- Outcome measurement
- Performance benchmarking
These tools help ensure that patients receive treatments that are proven to be effective.
2. Patient Safety
Patient safety is central to clinical governance. Healthcare organizations must implement systems to prevent harm and reduce medical errors. This includes:
-
- Incident reporting systems
- Root cause analysis
- Safety culture initiatives
- Learning from adverse events
A strong safety culture encourages staff to report errors and near misses without fear of blame.
3. Patient Engagement
Patients play an essential role in clinical governance. Patient engagement includes:
-
- Shared decision-making
- Patient feedback systems
- Patient representation in committees
- Transparent communication
Engaged patients contribute valuable perspectives that help improve healthcare quality.
4. Quality Improvement
Continuous improvement is a fundamental part of clinical governance. Healthcare organizations and professionals use quality improvement methods such as:
-
- Plan-Do-Study-Act (PDSA) cycles
- Process redesign
- Patient pathway optimization
- Performance monitoring
These activities enable organizations to refine systems and professionals to improve clinical outcomes over time.
5. Professional Development
Maintaining high standards of care requires ongoing education and training. Clinical governance therefore promotes:
-
- Continuing professional development
- Competency assessment
- Clinical supervision
- Interprofessional teamwork
By investing in workforce development, healthcare organizations strengthen their clinical capabilities.
Financial Governance: Responsible Resource Allocation
The second foundational pillar at the base of the governance pyramid is Financial Governance. Financial governance ensures that healthcare organizations use their resources responsibly, efficiently, and transparently. Healthcare systems operate under significant financial constraints. Effective financial governance ensures that resources are used to maximize health outcomes while maintaining organizational sustainability. Key elements of financial governance:
1. Financial Accountability
Healthcare organizations must maintain clear accountability for financial decisions. This includes:
-
- Transparent budgeting processes
- Financial reporting
- Internal controls
- Audit mechanisms
These systems protect the organization from fraud, mismanagement, and inefficiency.
2. Strategic Resource Allocation
Financial governance supports strategic decision-making by ensuring that resources are directed toward priority areas. Examples include:
-
- Investment in patient safety initiatives
- Infrastructure development
- Workforce training
- Digital health systems
By aligning financial decisions with organizational goals, healthcare organizations can improve both efficiency and patient outcomes.
3. Financial Sustainability
Long-term sustainability is essential for maintaining healthcare services. Financial governance supports sustainability through:
-
- Cost management
- Revenue planning
- Financial risk assessment
- Long-term investment planning
Healthcare leaders must balance cost control with the need to maintain quality care.
4. Value-Based Healthcare
Modern healthcare systems increasingly focus on value rather than volume. Financial governance supports this transition by promoting:
-
- Cost-effectiveness analysis
- Outcome-based funding models
- Efficiency improvements
- Waste reduction
These approaches ensure that resources are used in ways that deliver the greatest health benefit.
Organizational Culture: The Binding Force
While board governance, clinical governance, and financial governance form the structural elements of the governance pyramid, organizational culture binds them together. Culture refers to the shared values, beliefs, attitudes, and behaviors that shape how people work within an organization. A culture that supports good governance principles is essential for the effective functioning of the governance pyramid
Principles of Good Governance Culture
A governance culture in healthcare should be grounded in several core principles.
-
- Transparency. Transparency promotes openness in decision-making and reporting. When information is shared openly, trust increases among staff, patients, and stakeholders.
- Accountability. Accountability ensures that individuals and teams take responsibility for their actions and outcomes. Clear accountability structures improve performance and reduce errors.
- Integrity. Integrity promotes ethical conduct and honesty in all organizational activities. Healthcare organizations must uphold high ethical standards to maintain public trust.
- Participation. Inclusive governance encourages participation from healthcare professionals, patients, and community representatives. Diverse perspectives strengthen decision-making.
- Learning and Improvement. A culture of learning encourages staff to continuously improve systems and practices. Mistakes are viewed as opportunities for learning rather than blame.
Governance Pyramid Integration
The effectiveness of the governance pyramid depends on integration between its levels.
-
- Board governance provides strategic leadership and oversight.
- Clinical governance ensures quality and safety in healthcare delivery.
- Financial governance ensures responsible management of resources.
When these elements are aligned, healthcare organizations can achieve:
-
- Better patient outcomes.
- Stronger financial performance.
- Improved staff engagement.
- Greater public trust.
Conversely, weaknesses in any part of the pyramid can undermine the entire governance system. For example:
-
- Poor board oversight may allow quality failures to go unnoticed.
- Weak clinical governance may compromise patient safety.
- Ineffective financial governance may lead to resource shortages.
Therefore, healthcare organizations must continuously strengthen all components of the governance pyramid.
Governance Pyramid Benefits
The governance pyramid offers several advantages as a conceptual framework.
-
- Clarity of Roles. It clearly distinguishes between strategic oversight and operational governance responsibilities.
- System Perspective. The model highlights the interconnected nature of governance components.
- Focus on Culture. By emphasizing organizational culture, the model acknowledges the human and behavioral dimensions of governance.
- Support for Accountability. The pyramid structure reinforces the importance of accountability at every level of the organization.
- Alignment with Healthcare Priorities. The model reflects the core priorities of healthcare organizations: patient safety, quality care, and financial sustainability.
Conclusion
Effective governance is essential for the success of healthcare organizations. The Governance Pyramid provides a clear and practical framework for understanding how different governance elements interact to support high-quality healthcare delivery. At the top, Board Governanceprovides strategic direction and oversight. At the base, Clinical Governance ensures the safety and quality of patient care, while Financial Governance ensures responsible and sustainable resource management. These components are bound together by an organizational culture grounded in the principles of good governance, including transparency, accountability, integrity, participation, and continuous improvement. When these elements function together harmoniously, healthcare organizations can deliver safe, effective, and sustainable care for the populations they serve. The governance pyramid therefore serves not only as a conceptual model but also as a practical guide for strengthening governance systems and promoting excellence in healthcare organizations.
Disclosure
This monograph is based on a lecture delivered to the Health Governance Diploma. The monograph lecture-derived text has been generated using AI and human edited to fit purpose and allocated space.